Review Article
Kalgoorlie Hospital, Western Australia 1895-1897, the First Five Months of Hospital Admissions, and Typhoid in the Gold Fields
Peter Stride*
University of Queensland School of Medicine 23 Aland St, Wavell Heights, Brisbane, Queensland 4012, Australia
*Corresponding author: Peter Stride, University of Queensland School of Medicine 23 Aland St, Wavell Heights,
Brisbane, Queensland 4012, Australia; E-mail: pjostride@gmail.com
Article Information: Submission: 15/07/2015; Accepted: 20/08/2015; Published: 26/08/2015
Copyright: © 2015 Stride P. This is an open access article distributed under the Creative Commons Attribution License,
which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly
cited.
Abstract
Lessons from history can assist in management today by avoiding errors of the past. Kalgoorlie is a remote city in the Goldfields of Western Australia
600kms east of Perth with a current population of about 30,000. When gold was discovered there in 1893, thousands of optimistic prospectors flocked
there before the development of any community infrastructure. A tent city and then a tent hospital developed, dealing with the problems inherent in remote
mining communities lacking clean water and sanitation. Bars, beer and brothels traditionally arrive soon after mining strikes in Australia. Trauma, violence,
typhoid and other infections including venereal diseases were common. The unusual feature is that the current Kalgoorlie Base Hospital archives records
of admissions and discharges dating back to 1896. The clinical details of the first 298 inpatients admitted between 1st December 1896 and 27th April 1897
are presented.
Introduction
Kalgoorlie, now known as Kalgoorlie-Boulder after Kalgoorlie
and Boulder communities joined, is a city in the Goldfields-Esperance
region of Western Australia, Australia, located 600 kilometres eastnorth-
east of Perth at the end of the Great Eastern Highway. The
name Kalgoorlie is derived from the Wangai word Karlkurla, meaning
“place of the silky pears”.
In January 1893, three prospectors, Paddy Hannan, Tom
Flanagan, and Dan O’Shea passing through the area noticed signs
of gold in the area, and stopped. By June 1893, Hannan had filed
a claim, and hundreds of men swarmed to the area, some pushing
wheelbarrows or riding wooden bicycles from Perth, in search of gold and the town of Kalgoorlie was born. The arrival of tens of
thousands of people before the development of infrastructure and
with unhygienic conditions, unclean water, and inadequate disposal
of waste rapidly led to an epidemic of typhoid or enteric fever as
it was also known. Working exposed to the Australian sun can be
extremely dehydrating, and today many labourers carry ten litres of
water per day.
The author (PS) while working in Kalgoorlie hospital experienced
temperatures up to 47 °C, and had a 19 year old male with no previous
renal disease admitted with a creatinine over 300 mmol/L in spite of
consuming five litres of water during a day exposed to the sun in
January. He responded to intravenous saline with full recovery within
24 h.
It was impossible over 100 years ago to find ten litres of clean
water as workers carry today, and the prevalence of typhoid increased
in very hot spells as in 1902 when a heat wave with shade temperatures
over 100 °C resulted in over 90 cases in the Kalgoorlie Hospital [1].
In 1895 a hospital opened, initially in tents, and subsequently
in more permanent buildings. Records are available in the hospital
archives dating back to 1896 of early admissions, two-thirds of
whom were suffering from enteric fever caused by clinically identical
infection with either of the water or food borne Salmonella enterica
serotypes Typhi and Paratyphi.
By 1898 the town population was 2,018 (1516 males and 502
females), increasing to 30,000 people in 1903, much the same as the
population of 31,107 at the 2011 census. The area with a population
exceeding 200,000 in the 1890s gained a notorious reputation
inhabited by gamblers, bandits and prostitutes. By 1902, the town
had 8 breweries, several brothels and 93 hotels, some still functioning
today as some of the finest examples of mining town architecture in
the world.
The mining of gold along with other metals remains a major
industry in Kalgoorlie today, employing a quarter of Kalgoorlie’s
workforce, and generating a significant proportion of its income. The
central gold field area, known as the Golden Mile, is thought to be
the richest square mile on Earth. Kalgoorlie was connected by rail to
Perth in 1896 and to Port Augusta in South Australia in 1917. A fresh
water pipeline bringing in fresh water from Perth opened in 1903.
The History of Typhoid
The Typhoid bacillus was first detected and identified in 1880 by
Karl Eberth and confirmed as the cause of the disease by Georg Gaffky
in 1884, but it is considered to have been the cause of many past
outbreaks of infection with associated high mortality, for example
the Athenian plague of 430BC, which killed a third of the population
including Pericles and the disease which wiped out the English
settlement of Jamestown, Virginia, USA in the early 17th century.
It is thought to have caused the death of over 80,000 soldiers in the
American Civil War.
The association of typhoid with poor sanitation and disposal of
sewage was well known by the 1890’s. Patrick Manson in his text
‘Tropical Diseases’ notes the frequency of the disease in Europeans
soon after arrival in unsanitary places in Asia, particularly from
drinking contaminated water [2]. He writes:-‘Similar testimony has
come from Australia, where typhoid has occurred in the back country
in lonely spots, hundreds of miles from fixed human habitation’
William Osler was the leading global medical authority when gold
was discovered in Kalgoorlie. His text ‘The Principles and Practice
of Medicine’ describes the diagnosis and management of typhoid at
the closing of the 19th century [3]. Osler acknowledges the work of
Eberth, Koch, and Gaffky in identifying the causative organism, ‘a
short, thick, motile bacillus with rounded ends which grows readily on
various nutritive media’. He considered that ‘In cities the prevalence of
typhoid fever is directly proportionate to the inefficiency of the drainage
and the water supply’. Osler noted that the mortality varied from 10-
30% in different outbreaks. Improved sanitation and vaccination
introduced late in the 19th greatly reduced mortality.
Diagnosis
Clinical features are not available from the Kalgoorlie Hospital
records and the accuracy of the diagnosis of typhoid is pivotal to this
paper. Osler [3] considered the presence of rose-coloured spots and
splenomegaly were key features on examination. Connor reported
rose spots in 5-30% of cases, (blanching erythematous maculopapular
lesions usually 2-4 mm in diameter) usually on the abdomen and
chest [4].
The history of a pre-febrile phase with headache, malaise,
bronchitis and anorexia, followed by a febrile illness with diarrhoea
was strongly suggestive of typhoid. Osler considered splenic puncture
to obtain a culture was rarely justified.
Management
In the pre-antibiotic era, Osler [3] believed medications were of
no avail and that careful nursing under an intelligent nurse was critical
in the management of seriously ill patients in the era also before
intravenous fluids. He advised a low residue diet predominantly of
milk with plenty of water, but alcohol only for weakness, high fever
or a weak pulse. Patients with a high fever over 102.5oF should be
immersed in a cold bath every three hours, and severe diarrhoea
was treated with starch and opium enemata. Acetate of lead and
opium were recommended for haemorrhage. Osler recognised that
neurological features, peritonism and heart failure, for which he
recommended alcohol and strychnine being uncertain of the benefits
of digitalis, indicated a poor prognosis.
The Kalgoorlie Hospital and typhoid in the goldfields
There were three phases in the development of a hospital in
Kalgoorlie in the 1890s, a funding and planning phase, the initial
tent hospital, and the finally a permanent construction with extant
archived patient records commencing about the date of opening the
initial buildings.
Planning:
By 1894, the citizens of Kalgoorlie perceived a need for their own
hospital, similar to the nearby Coolgardie Hospital opened the previous
year. A meeting at the Exchange Hotel was proposed in December 1894
to commence fund raising, initially with a sports event [5].Motivated citizens with various relevant skills were gathered into a
committee to drive the construction and opening of this establishment,
which would be initially under canvas. They considered that the
building should be constructed of stone similar to the Coolgardie
Hospital, and that the State Government should pay the costs as they
had in providing hospitals for the citizens of Perth. The hospital doctor
requested that a portion of the miners subscriptions to the hospital
should be handed over to him as extra salary, but the committee
replied they “cannot entertain his proposal [6].”
The Tent Hospital
Kalgoorlie Hospital opened in canvas tents by March 1895, with
Ms Alerdice as the first matron. Prior to the opening a temporary
structure known as Hannan’s hospital received a few patients [7].
In September a miners’ public clinic between 1000 and 1100 hours and again between 1900 and 2000 hours was commenced. The
committee requested a district sanitary inspector and an improved
water supply from the Government to reduce water-borne diseases
among the rapidly increasing population.
Fortnightly fund raising smoke concert were organised, and the
positions of hospital medical officer with private practice for £200 per
annum, and of a matron, for £151 per annum with free quarters were
advertised [8].
In an era before mass production of cigarettes and the obvious
adverse effect of tobacco, the hospital doctor, Dr. O’Mahon, presided
over a well-attended concert and smoke social in Waldack’s Club to
raise funds for the Kalgoorlie Hospital [9].
Miss Bessie Way, daughter of Dr. E. W. Way, honorary surgeon
and board member of the Adelaide Hospital, and niece of the deputy
Governor of South Australia Chief Justice Way, successfully applied
for the position of matron. She was described as a highly accomplished
nurse following the best possible training at the Adelaide Hospital
[10,11].
Little information about typhoid in the Kalgoorlie district is
available before 1896, but Dr Barber reported three deaths from
typhoid in six months between August 1895 and February 1896,
and then a slight increase in the mild cases of typhoid admitted to
the Kalgoorlie hospital in January. With unfortunate and erroneous
optimism saw no reason to anticipate any serious outbreak of typhoid
in the district [12].
In February 1896, the tent hospital had 24 beds. The hospital
organisation was criticised in the local paper when four patients were
refused admission due to the lack of available beds, in spite of the
apparent availability of four other large tents which could have been
erected immediately [13]. In March 1896 the Works Department
accepted a tender to erect hospital tents containing thirty extra beds.
The tents were made of navy canvas erected under a single iron roof
to shelter nursing staff passing from ward to ward [14].
In March 1896, a Mr Geoghegan complained to the local
newspaper about a gentleman refused hospital admission without
medical review in spite of severe pain. Dr J.A. O’Meehan, the R.M.O.
defended his patient care by responding that the complaint was
somewhat exaggerated as the patient had a boil on his leg requiring
outpatient treatment. O’Meehan stated that the hospital was open
for public inspection on specified afternoons, an idea which could
be adopted today [15]. Enteric fever became more prevalent during
February when Dr. O’Meehan reported 24 admissions suffering from
typhoid with one death, amongst a total of 41 admissions with five
deaths [16].
Bishop Gibney stated that the new St. John of God Kalgoorlie
Hospital building would be open at all hours of the day and night
for urgent admissions regardless of creed and that clergyman of all
denominations would have free access to their parishioners [17].
Clergymen were not immune from illness and the Rev A. J. Burt was
reported to be improving in December 1986 after a long admission
[18], and similarly, Father Deasy was approaching discharge in April
1897 also after a long illness in the Kalgoorlie Hospital [19].
By April 1896, Kalgoorlie Hospital had 56 beds, with proposals
for another 34. The risk to hospital staff of catching diseases was
demonstrated in April 1896, when both Dr. O’Meehan, the hospital
medical officer, and Miss Bessie Way, the matron, contracted
typhoid. Clearly the position of matron was not an office job then.
Dr. O’Meehan recovered uneventfully and was expected to return
to work shortly, while Dr. Barber worked as locum medical officer.
Bessie Way was not admitted suggesting a mild attack. She returned to
her home in Adelaide by coach to Albany, then steamer to Adelaide,
for a month’s convalescence accompanied by her mother, who had
nursed in her daughter’s place and ‘moved about in the sick wards like
a ministering angel’
The typhoid epidemic worsened in April. 64 of the 76 patients
admitted had typhoid, which caused five of the seven deaths. The
Colonial Secretary approved Dr. J Barber’s telegram request for
another ward, but it was not erected as the outbreak subsided for a
while [20,21]. Soon after Bessie Way’s return, she became engaged to
Mr. Harvey, of Kalgoorlie, which then necessitating her retirement
from nursing, and Miss C. H. Bucklay was appointed as matron of the
Kalgoorlie Hospital [22,23].
In spite of cooler weather, typhoid caused 96 of the 113 admissions
plus four of the six deaths in June 1896, and 18 of the 36 admissions,
plus seven of the eight deaths in July in Kalgoorlie Hospital [23,24].
By October, plans for the new hospital were well advanced and Dr.
O’Meehan visited Perth for a few days to give an expert medical
opinion, then considered important in the construction of a new
hospital [25].
Records, currently archived in the Kalgoorlie Hospital, of
admissions to the Hospital date from December 1st1896. This paper
reviews the first 298 patients admitted between that date and April
27th 1897, with the last of the being discharged on 3rd September 1897
after 101 days in hospital. The tent hospital had been open at least
since late 1895 and some details are available in local papers, the more
permanent structure was opened about February 1897, though the
date is not clear.
The Permanent Building
Construction of the St. John of God’s Hospital building to replace
the tent hospital commenced in late 1896, and by January 1897 had
progressed sufficiently to anticipate the admission of patients within
three weeks. The paper reported ‘The front set of rooms, comprising
the sisters’ quarter’s, a reception-room, the kitchen and the scullery,
the washhouse, &c., is rapidly approaching the final stage. The sisters’
rooms are thoroughly ventilated in the walls and ceilings. They have
fire places, and are painted and papered in a. refreshing tint, with a
dado of fluted iron, a wooden skirting, and a bordering of wood. The
ceiling is of fluted iron also. The building alone will cost about £3,800,
and the framing will need an expenditure of between £40 and £500’
[26].
Three miners’ deaths in the Kalgoorlie Hospital were reported
in February and recorded in the admissions and discharges. One of
them Michael O’Grady, was admitted with typhoid on 22/1/1897 and
died six day later [27].
The co-located Mrs. Mecham’s Kalgoorlie Private Hospital, was
first mentioned when destroyed by fire! The fire broke out in a bush
shed an evening in March about 7 o’clock where one of the nurses
was lighting a lamp, unfortunately igniting the shed. The fire then
advanced too rapidly to prevent its progress. The eighteen patients in
the building at the time, all suffering from typhoid, were all evacuated
and safely transferred to the Government Hospital. The only
significant injury was to the recently arrived police constable Baxter’s
spine through a fall over a log of wood, and he was also conveyed to
the Hospital [28].
The new Kalgoorlie Hospital was visited by the state Premier, who
was subsequently farewelled with hearty cheers at the railway station,
presumably for his attendance, rather than his departure [29,30]. The
Dispensers J. Boilean & Co were awarded the pharmacy position in
the new hospital building.
The current Perth based principal medical office, Dr. Lovegrove,
paid an official visit to Kalgoorlie hospital in July 1897. Dr Lovegrove
supported the hospital doctor in public health issues [31]. In August
1897, Miss Lee, previously matron of the Coolgardie Hospital, became
matron of the Kalgoorlie Hospital [32].
Between December 1st, 1896 and April 27th 1897, 195 out of
298 (65%) admissions to Kalgoorlie Hospital had typhoid with 34
deaths (mortality rate 17%). 38% of these cases were miners, and 15
were involved in the preparation or distribution of food and drink,
as storekeeper (2), butcher (2), baker (2), house keeper, brewer,
hotel servant, cellarman, barman, brewer, housemaid, cordial
manufacturer and domestic, and therefore a serious risk factor in the
dissemination of the disease. 18 other patients were admitted with the
diagnosis of diarrhoea, dysentery and peritonitis, some of whom may
also have had typhoid. Two patients with typhoid were suspected of
having intestinal perforation, both died. The only nurse admitted to
Kalgoorlie hospital in the study period was Emily Herbert, aged 25,
with influenza for 12 days followed by uneventful discharge.
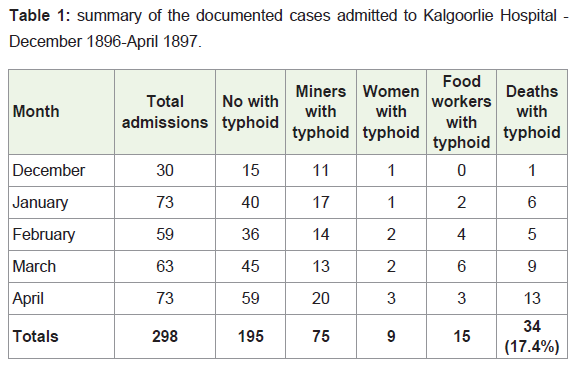
Table 1: summary of the documented cases admitted to Kalgoorlie Hospital - December 1896-April 1897.
After the initial typhoid epidemics swept the goldfields no
subsequent epidemic disease had such a serious impact. Other
common infections at the time included influenza, bronchitis,
tuberculosis and meningitis, and there were also many admissions
with trauma sustained in the mines and elsewhere.
Fresh water and Charles O’Connor
Kalgoorlie finally obtained a fresh water supply, pumped from
Perth thanks to the vision and engineering expertise of an Irishman
Charles O’Connor. He became Engineer-in-Chief of Western
Australia in 1891. He is best known for the construction of Freemantle
harbour, but the construction of a pipeline from Mundaring Weir
near Perth was a unique feat in engineering at that time. Forrest the
premier approved a loan of £2.5 million. 5 million imperial gallons
was pumped in eight successive stages through 530 km of 760 mm
diameter pipe to Kalgoorlie. Unfortunately O’Connor was criticised
in parliament and the media as incompetent and corrupt, resulting
in his suicide a month before the pipe commenced sending water to
Kalgoorlie. A subsequent inquiry belatedly cleared him of any wrong
doing. O’Connor, an expert professional, was politically naive and
unaccustomed to the mud-slinging of politicians. Today his vision
and skill are recognised and an electorate in Western Australia is
named after him [33].
Kalgoorlie Hospital today
Kalgoorlie Hospital, the largest regional public hospital in Western
Australia is a 131-bed inpatient facility, with a 24 h Emergency
Department servicing over 20,000 patients per year, a coronary care/
high dependency unit, a dialysis unit plus medical, surgical, obstetrics
and gynaecology, paediatric, mental health, and orthopaedic wards.
Sub-specialists in ENT, Urology, Ophthalmology and Oncology visit
regularly and the Royal Flying Doctor is available to take complex
and critical cases to tertiary hospitals in Perth. Trauma from motor
vehicle accidents and mining injuries and alcoholism are common.
Past terminology:
Some terms appear in the ‘designation’ or diagnostic column
that are no longer in common usage. Morbus cordis means heart
disease, possibly heart failure, but usually used when a more specific
diagnosis is not clear; phthisis specifically meaning wasting, but
used almost specifically for tuberculosis: cholera nostras is an illness
similar to cholera: ptomaine poisoning means food poisoning by a
microorganism, simple continuous fever means exactly that, a nonspecific
term still found in homeopathy texts, and capillary bronchitis
is now termed bronchiolitis.Typhoid in the 21st century:
Typhoid, or enteric fever, remains a severe global problem
compounded by increasing antibiotic resistance, limited vaccine
efficacy and international tourism today with an estimated 22 million
cases annually and an estimated 200,000 - 600,000 deaths [34]. In the
twenty-first century enteric fever has largely become a disease of the
third world where standards of water cleanliness and sanitation are
suboptimal. It is found mainly in Asia where an estimated 13 million
cases occur annually, with 400 000 deaths, particularly following war
or natural disasters where water supplies become polluted. Children
have disproportionately increased levels of morbidity and mortality.Chloramphenicol, Ampicillin, and Co-trimoxazole have been
used to treat typhoid since they first became available, however
Chloramphenicol resistance had become widespread forty years ago,
and resistance to all three has been detected in Asia for over twenty years. Flouroquinalones have become the drug of choice. Current
vaccines are ineffective against S. paratyphi, the predominant tourists’
pathogen, and provide only moderate protection against S. Typhi [4].
In first world counties, typhoid has become a disease of young
unvaccinated tourists to Asia. Improvements in sanitation and
hygiene between 1920 and 1990 reduced the annual number of cases
in USA from about 36.000 to approximately 500. The proportion
acquired during foreign travel over the thirty years between 1967 and
1997 has increased from 33% to 81% [4].
Lynch reported 1902 typhoid fever cases, median age 22 years,
detected in USA between 1999 and 2006, 1295 (73%) required
hospitalization and 3 (0.2%) died. 1439 (79%) reported foreign
travel in the previous 30 days of illness, only 58 travellers (5%) had
been vaccinated against typhoid. 272 (13%) of 2016 isolates tested
were resistant to ampicillin, chloramphenicol, and co-trimoxazole
(multidrug-resistant S Typhi) [35].
Enteric fever still occurs in Australasia. Auckland Hospital
reported 162 confirmed cases in a six year period, 50% having
travelled beyond the Pacific area, 25% had travelled within the Pacific
and 25% had not left New Zealand. 83% were Salmonella typhi. Fever
and diaphoresis were reported by 91% of patients, but only 61% had
diarrhoea. Ciprofloxacin and amoxicillin were the most commonly
prescribed antibiotics. The median length of stay was six days
compared with 50 days a hundred years ago and there were no deaths
compared with 17% in the gold rush days of Kalgoorlie. However 28%
of the New Zealand cases had a recent previous admission to hospital
with probable typhoid when the correct diagnosis was not made,
probably a higher figure than in early Kalgoorlie where familiarity
would generate a higher level of suspicion.
Conclusion
Enteric fever caused most of the admissions and deaths in
the Kalgoorlie hospital in the early days of the gold rush 120 years
ago. In spite of the advances since then, the disease remains a very
common cause of essentially preventable morbidity and mortality in
a world where first world greed and labels appear more important
than providing a safe supply of water in the third world. The third
world needs a Charles O’Connor! The problem will be increasingly
exacerbated by progressive antibiotic resistance and the limited
efficacy of current vaccines unless we act soon to ensure safe water
all over the world.
References
Citation
Stride P. Kalgoorlie Hospital, Western Australia 1895-1897, the First Five Months of Hospital Admissions, and Typhoid in the Gold Fields. J Environ Soc Sci. 2015;2(2): 116.